Research
Cost-Driver Medications in the Top California Workers' Comp Drug Groups: Part 2, Dermatologicals, Opioids, and Antidepressants
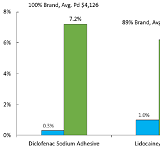
The second in a 3-part research series on workers' compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part 2 of the series focuses on Dermatologicals, Opioids, and Antidepressants.
CWCI Report to the Industry Examines Factors that Drive IMR Volume and Outcomes
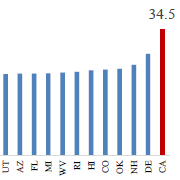
A new CWCI Report to the Industry provides an in-depth look at the dispute resolution process in California workers compensation and examines IMR activity and outcomes from 2014 through 2022.
Cost-Driver Medications in the Top California Workers' Comp Drug Groups: Part 1, Anti-Inflammatories & Anticonvulsants
The first of a 3-part research series on workers' compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part I of the series focuses on Anti-Inflammatories and Anticonvulsants.
Patterns in the Provision of Professional Medical Services in California Workers Compensation
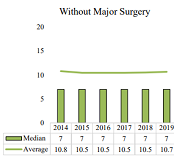
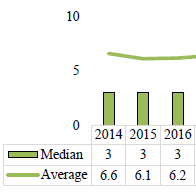
CWCI research tracks changes in the prevalence and volume of professional medical services in the first 2 years of treatment for indemnity claims in which medical care began between 2014 and 2019. To examine the impact of the pandemic, the authors compare the prevalence and volume of services in the first 6 months of treatment for claims in which treatment began in 2018 and 2019 claims in which treatment began in 2020 and 2021. In both cases, results are broken out for claims with and without surgery.
Trends in the Utilization of Inpatient Care in California Workers' Compensation
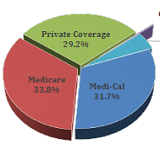
A Research Update report that continues CWCIs series of studies examining inpatient utilization trends using data compiled by the California Department of Health Care Access and Information. The analysis compares the volume and types of inpatient hospitalizations covered by workers compensation to those covered by Medicare, Medi-Cal, and private coverage.
Underlying Issues and Outcomes in Reducing the Compensability Determination Timeline
In both 2021 and 2022, California legislators have debated proposals that would shorten the compensability determination timeline for California workers compensation claims. This CWCI Impact Analysis report helps bring the debate into focus by providing background information on the compensability determination process for litigated and non-litigated claims, reviewing existing statutory and regulatory timeframes for various steps within the process, and using data from nearly 460,000 non-COVID-19 claims and more than 17,000 COVID-19 claims to evaluate the need for and the potential impact of the proposals, including the unintended consequences.