Research
CWCI Analysis of California WC Inpatient Care, 2012-2022
A CWCI Research Update report uses HCAI data to monitor trends in the utilization of inpatient care in California workers comp from 2012 through 2022, comparing the workers comp trends to those in Medicare, Medi-Cal and private coverage. The report also reviews changes in the types of conditions treated and the services delivered to injured workers before and after the pandemic was declared in 2020; takes a focused look at the primary diagnoses underlying inpatient hospitalizations involving spinal fusions and major joint replacement surgeries; and examines how the growth of outpatient surgery is affecting the total number of injured worker hospitalizations.
Analysis of Cumulative Trauma & Litigated Claims in California Workers' Comp
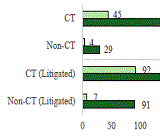
CT & Litigated Claims in California Workers' Comp. A CWCI Research Note based on 1.4 million claims with claims administrator notification dates ranging from 2010 through 2022 tracks the growth of CT claims in California workers' compensation and examines the impact that factors such as region, tenure, industry, age, and average weekly wage have on the likelihood of CT claims.
Claims Monitoring: Medical and Indemnity Development, AY 2013 – AY 2022
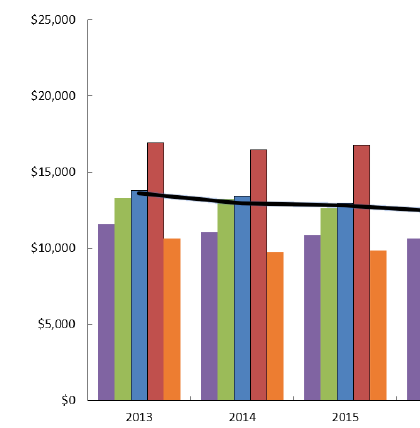
A CWCI analysis of data from the IRIS database tracks average California workers' comp total losses per indemnity claim since the implementation of SB 863 through the first three years of the pandemic, and breaks out the data to show both paid medical and paid indemnity loss trends. The study also looks at 24-month loss trends for claims from five key industry sectors and for claims from injured workers living in 7 distinct regions of the state as well as from workers living out of state.
An Early Look at the Impact of the New Med-Legal Fee Schedule
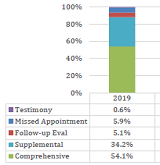
CWCI research takes an in-depth look at the impact of the Med-Legal Fee Schedules revised reimbursement rules and fees by comparing various utilization and payment metrics from before and after the schedule took effect on April 1, 2021. Read the full report.
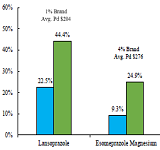
Cost-Driver Medications in the Top California Workers' Comp Therapeutic Drug Groups: Part 3, Musculoskeletal and Ulcer Drugs
The final report in a 3-part research series on workers' compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part 3 of the series focuses on Musculoskeletal and Ulcer Drugs.
An Analysis of AB 1213's Proposed Change to the 104-Week TD Cap
CWCI examines a proposal to alter the TD cap by excluding TD that is paid or due from the UR treatment denial date to the date of the treatment authorization if the denial is overturned by IMR or the WCAB. The analysis estimates the percentage of claims that would be affected by the proposal in light of the required IT costs to update claims systems and the ongoing administrative costs for manual processes to identify and track claims with TD payments and UR and IMR activity.