Research
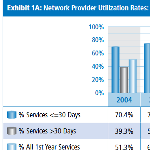
Use of Network Physicians in California WC, AY 2004-3Q2011 Claims
The latest research on network provider utilization in California workers’ compensation shows network physicians delivered nearly 80% of first-year, physician-based outpatient treatment on AY 2010 claims.
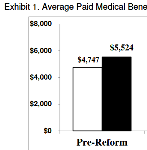
Differences in Outcomes for Injured Workers Receiving Physician-Dispensed Repackaged Drugs in the California WC System
New CWCI Research shows California workers’ comp claims that involve physician-dispensed repackaged drugs have higher average medical and indemnity payments and more days away from work than comparable claims with no physician-dispensed repackaged drugs.
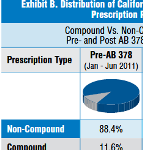
Current Trends In Compound Drug Use and Costs in California WC
New CWCI research shows compound drugs accounted for a declining share of prescription medications dispensed to California injured workers last year, yet compound drug payments continued to represent a growing percentage of prescription dollars.
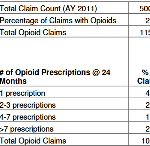
Estimated Savings from Enhanced Opioid Management Controls through 3rd Party Payor Access to the Controlled Substance UR and Evaluation System (CURES)
A new Institute analysis suggests that allowing workers’ comp payers access to data from the state’s prescription drug monitoring program (CURES) would help reduce inappropriate dispensing of opioids in workers’ comp, improving injured worker treatment and saving an estimated $57 million in AY 2011 claim costs.
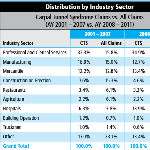
ICIS Injury Score Card: Carpal Tunnel Syndrome
CWCI’s latest injury score card provides detailed data on California workers’ compensation carpal tunnel claims from accident years 2001 through 2011.
Medical Development Trends in California WC, AY 2002-2011 Claims
Updated figures from CWCI research show continued growth in average amounts paid for medical services in California workers’ comp, with payments for treatment, prescriptions and durable medical equipment, med-legal reports and medical management all trending up.