Research
IMR Decisions: January 2014 Through December 2016
A 12-page CWCI analysis that measures and compares IMR outcomes from 2014, 2015, and 2016.
Cumulative Trauma in California WC
A new CWCI study provides a detailed data on California workers compensation cumulative trauma (CT) claims, identifies characteristics that differentiate CT claims from non-CT claims, and finds the high cost of CT claims is strongly associated with high levels of attorney involvement and the high incidence of CT claims in the L.A. Basin.
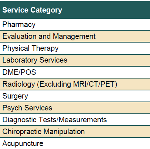
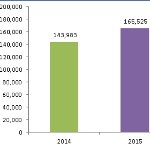
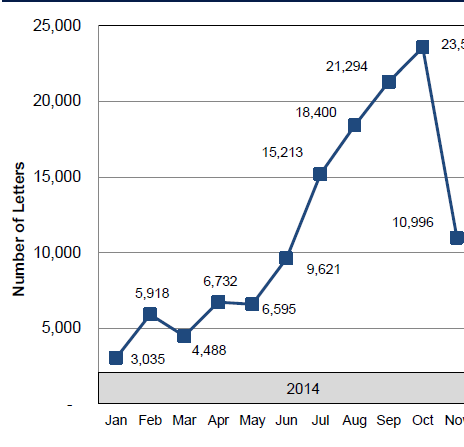
Independent Medical Review Decisions – January Through December 2015
A detailed analysis on IMR outcomes, including decision counts and uphold rates, based on data gleaned from 2015 IMR determination letters
Medical Review and Medical Dispute Resolution in California WC
New CWCI research based on 2014 UR data and IMR determinations from the first half of 2015 shows an estimated 96 percent of medical services in California workers' comp are approved.
Prescribing Patterns for Schedule II Opioids in Calif. WC.
A new CWCI study on prescribing patterns for Schedule II Opioids in California workers' compensation finds that a relatively small percentage of medical providers account for the vast majority of these narcotic prescriptions and the associated payments, and that more than half of the prescriptions are for minor back injury claims.
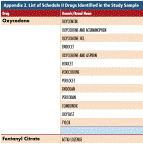
Prescribing Patterns of Schedule II Opioids Part 2: Fentanyl Prescriptions in California Workers' Compensation
A CWCI Research Spotlight Report on the use of fentanyl – the most potent Schedule II opioid – in California workers' comp finds that more than 1 out of every 5 injured workers who are prescribed Schedule II opioids receive fentanyl, while more than a quarter of all claimants with non-surgical medical back problems who are prescribed Schedule II opioids receive fentanyl.