Research
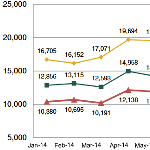
California WC Independent Medical Review: 1st Quarter 2015 Outcomes
An analysis of 2015 independent medical review (IMR) decisions from the first quarter of 2015 shows no significant decline in IMR volume in the first three months of this year, even though the independent medical reviewers continue to concur with the utilization review (UR) physicians denial or modification of treatment in about 90 percent of the cases.
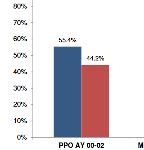
PPO to MPN: Impact of Physician Networks in California WC
A new CWCI study examines changes in the use of physician networks in California workers’ comp from AY 2000 – June AY 2011, measures their impact on medical costs and compares the changing nature and characteristics of claims where treatment is managed inside and outside of networks.
IMR Outcomes in California Workers Comp
A CWCI analysis of 2014 IMR decisions suggests that the medical dispute resolution process mandated by SB 863 is working to assure that treatment provided to California injured workers meet evidence-based medicine standards and is providing a needed check against unnecessary and potentially harmful tests, surgeries, drugs and procedures.
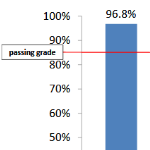
California WC Claims Administrator UR Audit Results: 2009 – 2013
A review of DWCs 2009-2013 UR audit results show claims administrators had an average performance rating of more than 97% over the 5-year period.
Ambulatory Surgery Center Cost Outcomes Follow-Up Study: The Impact of SB 863 WC Reforms
Average facility fee payments to ambulatory surgery centers have declined 27% per episode and 29% per procedure since ASC fee schedule changes mandated by SB 863 were adopted in 2013. Click here for the full report published jointly by CWCI and the WCIRB.
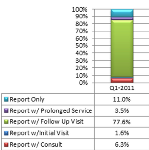
Changes in WC Physician Reporting Under the RBRVS Fee Schedule: Initial Results
The average amount paid for all California WC physician reports fell 37% from $26.13 in the 1st quarter of 2013 to $16.53 in the 1st quarter of 2014 as the state began to transition to the new RBRVS Fee Schedule, but that decline was due to changes in the underlying E&M services in the schedule and not a decrease in the fee schedule amounts assigned to report codes.