Research
Benchmark Data on Physician Reporting in California Workers' Comp Prior to Adoption of the RBRVS Physician Fee Schedule
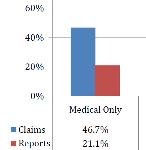
A new CWCI study finds that the average number of medical reports per claim provided by California workers comp treating physicians to claims administrators rose steadily for more than a decade prior to the adoption of the RBRVS fee schedule, fueled in part by increases in the average number of E/M services per claim and in the number of physician reports per E/M service, but claims organizations note that reports still dont always meet regulatory requirements or include all of the information needed for effective claims management.
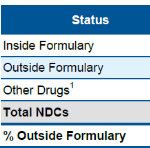
Are Formularies a Viable Solution to Controlling Prescription Drug Utilization and Cost in California WC?
A new CWCI study assesses the potential impact of a state-mandated drug formulary in California Workers' Compensation.
California Workers Compensation Medical and Indemnity Benefit Trends, AY 2002 – 2014
A new CWCI study monitors the growth in California Workers' Compensation medical and indemnity payments from accident year 2002 to accident year 2014.
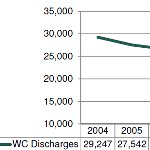
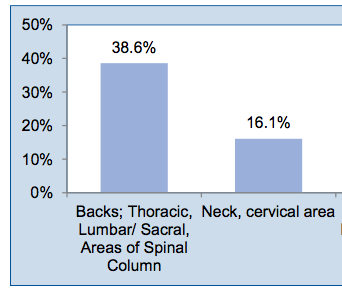
CWCI Study Documents Changes in Calif WC Inpatient Hospital Utilization and Implant-Eligible Spinal Surgeries
CWCIs latest study tracks inpatient hospital utilization trends, monitors changes in the use of implant-eligible spinal surgeries and estimates the savings from eliminating pass-through payments for spinal surgery hardware.
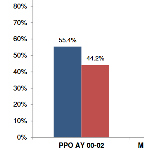
PPO to MPN: Impact of Physician Networks in California WC
A new CWCI study examines changes in the use of physician networks in California workers' comp from AY 2000 – June AY 2011, measures their impact on medical costs and compares the changing nature and characteristics of claims where treatment is managed inside and outside of networks.
Opioids in Workers' Compensation Medicare Set-Asides
CWCIs analysis of the prevalence and cost of prescription drugs within approved Workers' Compensation Medicare Set-Aside Arrangements.