Research
California Workers' Compensation Medical Payments, Litigation, and Claim Duration A Post-Reform Report Card
The Institute has published a report on a study linking increased litigation, claim duration and medical payments to judicial, legislative and regulatory changes implemented in the three years following enactment of the 1993 California workers compensation reforms.
Revisiting 24-Hour Health Care Coverage and Its Integration With the California Workers' Comp System
A CWCI white paper that examines the issues, opportunities, and unresolved problems surrounding the integration of California workers' comp into a 24-hour system.
Changes in the QME Population and Medical-Legal Trends in California Workers' Compensation
This study tracks changes in the composition of the Qualified Medical Evaluator (QME) population in California workers' compensation in terms of medical specialty representation and geographic availability, comparing data on medical providers certified as QMEs in 2012 and in 2017. The study also uses 2007 – June 2017 claims data to examine changes in the level of services rendered by evaluators, the mix of services, average payments for all medical-legal services and for specific levels of service, and the proportion of evaluations performed by AMEs vs. QMEs.
Schedule II Prescription & Payment Distributions in California WC: 2005 – 2008
California workers' compensation law provides that injured workers are entitled to all reasonable and necessary medical care to cure or relieve the effects of a work-related injury or illness.
Clinical Severity in Workers' Compensation Inpatient Care
This Research Abstract measures differences in inpatient admission characteristics, hospital resource use and clinical severity between California's workers compensation, group health and Medicare systems. The results challenge the perception that workers compensation admissions are "more difficult" to treat than patients from other systems.
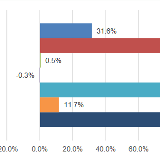
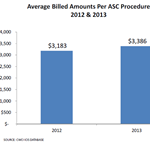
CWCI/WCIRB Study Finds Average ASC Facility Fee Payments Down 26 to 28 Percent Under Revised Fee Schedule
Preliminary data show average facility fee payments to ambulatory surgery centers have declined 26 percent per episode and 28 percent per procedure since fee schedule revisions took effect January 1, 2013.