Research
The Utilization of Physical Medicine in California Workers Comp Following Implementation of Mandatory UR and 24-Visit Caps
The goal of this physical therapy and chiropractic manipulation analysis was to determine any emerging correlations between the implementation of the utilization review program effective January 1, 2003, the 24-hour visit vap effective on January 1, 2004 and changes in the average utilization and cost of these services.
Changes in Outpatient Surgery Payments Following Adoption of the Outpatient Surgery Facility Fee Schedule
This analysis compared the average amounts paid under the revised outpatient surgery facility fee schedule effective on January 1, 2004 to the average payments for the same services prior to adoption of the schedule.
Measuring the Value of Medical Treatment Outside ACOEM Guideline Targets on Low Back Soft Tissue Injury Outcomes
This study compares recovery and cost outcomes and the use of common medical procedures 1) not recommended by the ACOEM Guidelines and 2) those recommended with optimal targets (PT and chiro services). Results show that when treatment exceeded ACOEM-recommended levels, medical and indemnity payments, treatment durations, and the number of paid TD days were significantly higher for many medical service categories.
Utilization Review & the Use of Medical Treatment Guidelines in California Workers Compensation
This study compares the evidence base and medical recommendations underlying different medical treatment guidelines for low back injury. The results show that different guidelines often have fundamentally different recommendations in regard to appropriate services and frequency of treatment for low back injuries — a lack of agreement that can produce conflict and debate within the workers compensation system.
An Analysis of Medical Utilization Trends
This report established baseline medical utilization data to begin to track trends subsequent to the inception of AB749.
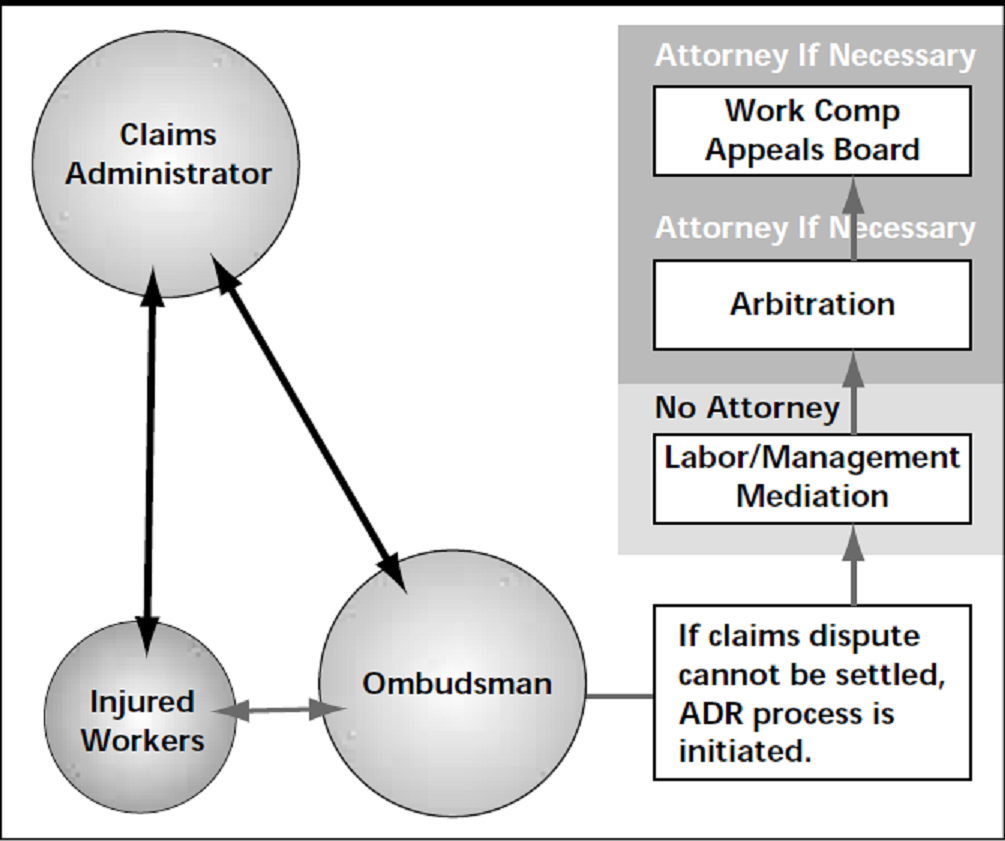
California WC ADR System: Attorney Involvement Rates and Claim Costs
A 9-page CWCI Report to the Industry details CWCI research that looks at the history of alternative dispute resolution programs (ADRs) in California workers compensation and compares attorney involvement and benefit payments for similar claims handled under ADRs and traditional workers compensation policies.