Research
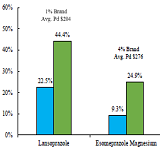
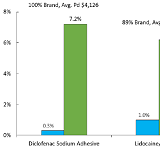
Cost-Driver Medications in the Top California Workers’ Comp Therapeutic Drug Groups: Part 3, Musculoskeletal and Ulcer Drugs
The final report in a 3-part research series on workers’ compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part 3 of the series focuses on Musculoskeletal and Ulcer Drugs.
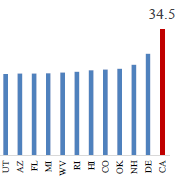
An Analysis of AB 1213’s Proposed Change to the 104-Week TD Cap
CWCI examines a proposal to alter the TD cap by excluding TD that is paid or due from the UR treatment denial date to the date of the treatment authorization if the denial is overturned by IMR or the WCAB. The analysis estimates the percentage of claims that would be affected by the proposal in light of the required IT costs to update claims systems and the ongoing administrative costs for manual processes to identify and track claims with TD payments and UR and IMR activity.
Cost-Driver Medications in the Top California Workers’ Comp Drug Groups: Part 2, Dermatologicals, Opioids, and Antidepressants
The second in a 3-part research series on workers’ compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part 2 of the series focuses on Dermatologicals, Opioids, and Antidepressants.
CWCI Report to the Industry Examines Factors that Drive IMR Volume and Outcomes
A new CWCI Report to the Industry provides an in-depth look at the dispute resolution process in California workers compensation and examines IMR activity and outcomes from 2014 through 2022.
Patterns in the Provision of Professional Medical Services in California Workers Compensation
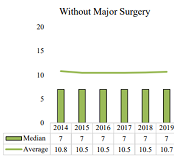
CWCI research tracks changes in the prevalence and volume of professional medical services in the first 2 years of treatment for indemnity claims in which medical care began between 2014 and 2019. To examine the impact of the pandemic, the authors compare the prevalence and volume of services in the first 6 months of treatment for claims in which treatment began in 2018 and 2019 claims in which treatment began in 2020 and 2021. In both cases, results are broken out for claims with and without surgery.
Cost-Driver Medications in the Top California Workers’ Comp Drug Groups: Part 1, Anti-Inflammatories & Anticonvulsants
The first of a 3-part research series on workers’ compensation medications that represent a relatively small share of the dispensed prescriptions within their therapeutic drug group, but due to their high average reimbursements, account for a disproportionate share of the total drug spend within their group. Part I of the series focuses on Anti-Inflammatories and Anticonvulsants.